How to Ensure That Your Infusion Pump Is Reliable
The FDA defines the external infusion pump as being "a medical device used to deliver fluids into a patient's body in a controlled manner". It is "capable of delivering fluids in large or small amounts, and may be used to deliver nutrients or medications – such as insulin or other hormones, antibiotics, chemotherapy drugs, and pain relievers. Some infusion pumps are designed mainly for stationary use at a patient’s bedside. Others, called ambulatory infusion pumps, are designed to be portable or wearable." More details on the infusion pump and its uses can be found on FDA's website.
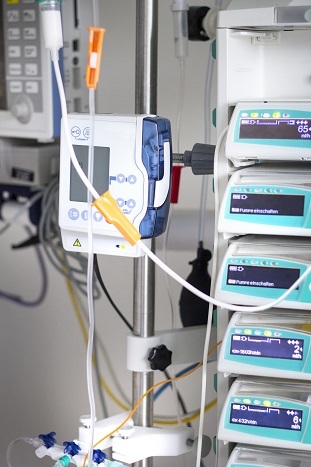
Costly Risks Associated With its Use
From 2005 through 2009, FDA received approximately 56,000 reports of adverse events associated with the use of infusion pumps, including numerous injuries and deaths. In 2017, ECRI Institute of Plymouth Meeting, Pennsylvania, named infusion errors as No. 1 on its annual list of healthcare technology hazards (source). The FDA has summarized the three major reasons for infusion pump malfunctions as the following:
1. Software Defects.
Some pumps fail to activate pre-programmed alarms when problems occur, while others activate an alarm in the absence of a problem. Other software errors can lead to over- or under-infusion. In one case, a software problem called a “key bounce” caused an infusion pump to occasionally register one keystroke (e.g., a single zero, “0”) as multiple keystrokes (e.g., a double zero, “00”).
2. User Interface Issues.
Numerous reports of confusing or unclear on-screen user instructions lead to improper programming of medication doses or infusion rates. For example, the design of the infusion pump screen may not make clear which units of measurement (e.g., pounds versus kilograms) should be used to enter patient data, leading to inappropriate dosing.
3. Mechanical or Electrical Failures.
Other problems reported include components, such as pump housings, that break under routine use; premature battery failures; and sparks or pump fires. Each of these types of incidents can create risks to patients, including the potential for over- or under-administration of critical fluids.
The most common battery failure, however? Human Negligence.
This includes batteries not being replaced during the recommended end of life routine maintenance, or when the patient themselves return from ambulating and forget to plug in the infusion pump, causing a low battery message and alarm to appear, usually too quiet to the point of going unnoticed.
Is there an easy solution?
Yes.
ECRI Institute argues that every one of the above issues is preventable, or at least can be mitigated with better technology management. For starters, electrical harms such as premature battery failures are arguably one of the easiest to fix if the correct technology is implemented. Currently, healthcare workers often have to send patients with two devices as there is a constant worry that one is going to fail during ambulance or hospital transport (source).
Not only does the C7400 ER Battery Analyzer keep hospital batteries charged and ready to go, but it enables you to keep track of your fleet, run quality reports, and label batteries using the Cadex PC-Batteryshop™ software. By implementing this system, the number of injuries educed by infusion pump failure can be greatly minimized.
Want to learn more about Healthcare Battery Maintenance? Cadex has published a 3-part e-book on the topic, which can be downloaded here.
